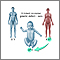
Duchenne muscular dystrophy is an inherited disease. It involves muscle weakness, which quickly gets worse.
Causes
Duchenne muscular dystrophy is a form of muscular dystrophy. It worsens quickly. Other muscular dystrophies (including Becker muscular dystrophy) get worse much more slowly.
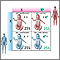
Duchenne muscular dystrophy is caused by a variant gene for dystrophin (a protein in the muscles). However, it often occurs in people without a known family history of the condition.
The condition affects boys due to the way the condition is inherited. The sons of women who are carriers of the condition (women with a variant gene, but no symptoms themselves) each have a 50% chance of having the condition. The daughters each have a 50% chance of being carriers. Very rarely, a female can have symptoms if they have the variant gene.
Duchenne muscular dystrophy occurs in about 1 out of every 3,500 male infants. Because this is an inherited disorder, risks include a family history of Duchenne muscular dystrophy.
Symptoms
Symptoms most often appear before age 6. They may start as early as infancy. Most boys show no symptoms in the first few years of life.
Symptoms may include:
- Fatigue
- Learning difficulties (the IQ can be below 75)
- Intellectual disability (possible, but does not get worse over time)
Muscle weakness:
- Begins in the legs and pelvis, but also occurs less severely in the arms, neck, and other areas of the body.
- Problems with motor skills (running, hopping, jumping).
- Frequent falls.
- Trouble getting up from a lying position or climbing stairs.
- Shortness of breath, fatigue, and swelling of the feet due to a weakening of the heart muscle.
- Problem breathing due to a weakening of the respiratory muscles.
- Gradual worsening of muscle weakness.
Progressive difficulty walking:
- Ability to walk may be lost by age 12, and the child will have to use a wheelchair.
- Breathing difficulties and heart disease usually start by age 20.
Exams and Tests
A complete nervous system (neurological), heart, lung, and muscle exam may show:
- Abnormal, weak heart muscle (cardiomyopathy) that becomes evident by age 10
- Congestive heart failure or irregular heart rhythm (arrhythmias) that is present in all people with Duchenne muscular dystrophy by the age of 18
- Deformities of the chest and back (scoliosis)
- Enlarged muscles of the calves, buttocks, and shoulders (around age 4 or 5). These muscles are eventually replaced by fat and connective tissue (pseudohypertrophy)
- Loss of muscle mass (wasting)
- Muscle contractures in the heels, legs
- Muscle deformities
- Respiratory disorders, including pneumonia and swallowing with food or fluid passing into the lungs (in late stages of the condition)
Tests may include:
- Blood creatine kinase levels
- Electrocardiogram (ECG)
- Cardiac testing
- X-rays of the spine to determine if there is a scoliosis
- Pulmonary function tests
- Electromyography (EMG)
- Genetic tests
- Muscle biopsy
Treatment
There is no known cure for Duchenne muscular dystrophy. Treatment aims to control symptoms to improve quality of life.
Steroid medicines can slow the loss of muscle strength. They may be started when the child is diagnosed or when muscle strength begins to decline.
Other treatments may include:
- Albuterol (to help with muscle strength)
- Amino acids
- Levocarnitine (L-carnitine)
- Coenzyme Q10
- Creatine
- Fish oil
- Givinostat
- Green tea extracts
- Vitamin E
However, the effects of these treatments have not been proven. Stem cells and gene therapy may be used in the future.
Genetic therapies may be helpful to certain people, depending on the genetic cause. Each therapy only works on a small number of people, depending on their specific genetic change. While these treatments have been shown to increase dystrophin production, they have not yet been shown to have significant clinical benefits.
Treatments include:
- Eteplirsen
- Golodirsen
- Vitolarsen
- Casimersen
- Ataluren
- Delandistrogene moxeparvovec
The use of steroids and the lack of physical activity can lead to excessive weight gain. Activity is encouraged. Inactivity (such as bedrest) can make the muscle condition worse. Physical therapy may help to maintain muscle strength and function. Speech therapy is often needed.
Other treatments may include:
- Assisted ventilation (used during the day or night)
- Medicines to help heart function, such as angiotensin-converting-enzyme inhibitors, beta-blockers, and diuretics
- Orthopedic appliances (such as braces and wheelchairs) to improve mobility
- Spine surgery to treat progressive scoliosis for some people
- Proton pump inhibitors (for people with gastroesophageal reflux)
Several new treatments are being studied in trials.
Support Groups
You can ease the stress of the condition by joining a support group where members share common experiences and problems. The Muscular Dystrophy Association is an excellent source of information on this condition.
Outlook (Prognosis)
Duchenne muscular dystrophy leads to progressively worsening disability. Death often occurs from lung disorders, although advances in supportive care have resulted in many men living to age 35 years.
Possible Complications
Complications may include:
- Cardiomyopathy
- Congestive heart failure (rare)
- Deformities
- Heart arrhythmias (rare)
- Mental impairment (varies, usually minimal)
- Permanent, progressive disability, including decreased mobility and decreased ability to care for self
- Pneumonia or other respiratory infections
- Respiratory failure
When to Contact a Medical Professional
Contact your health care provider if:
- Your child has symptoms of Duchenne muscular dystrophy
- Symptoms get worse, or new symptoms develop, particularly fever with cough or breathing problems
Prevention
People with a family history of the condition may want to seek genetic counseling. Genetic studies done during pregnancy are very accurate in detecting Duchenne muscular dystrophy.
Alternative Names
Pseudohypertrophic muscular dystrophy; Muscular dystrophy - Duchenne type
References
Doughty CT, Amato AA. Disorders of skeletal muscle. In: Jankovic J, Mazziotta JC, Pomeroy SL, Newman NJ, eds. Bradley and Daroff's Neurology in Clinical Practice. 8th ed. Philadelphia, PA: Elsevier; 2022:chap 109.
Genetic and Rare Diseases Information Center (GARD). Duchenne muscular dystrophy. rarediseases.info.nih.gov/diseases/6291/duchenne-muscular-dystrophy. Updated December 2025. Accessed December 19, 2025.
Lee BH. The Dystrophinopathies. Continuum (Minneap Minn). 2022;28(6):1678-1697. PMID: 36537975 pubmed.ncbi.nlm.nih.gov/36537975/.
Manzur AY. Muscular dystrophies. In: Kliegman RM, St. Geme JW, Blum NJ, et al, eds. Nelson Textbook of Pediatrics. 22nd ed. Philadelphia, PA: Elsevier; 2025:chap 649.
Muscular Dystrophy Association website. Duchenne muscular dystrophy (DMD). www.mda.org/disease/duchenne-muscular-dystrophy. Accessed December 19, 2025.
Selcen D. Muscle diseases. In: Goldman L, Cooney KA, eds. Goldman-Cecil Medicine. 27th ed. Philadelphia, PA: Elsevier; 2024:chap 389.
Review Date 10/27/2025
Updated by: Joseph V. Campellone, MD, Department of Neurology, Cooper Medical School at Rowan University, Camden, NJ. Review provided by VeriMed Healthcare Network. Also reviewed by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.