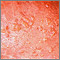
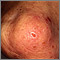
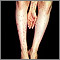
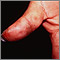
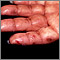
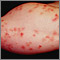
Dermatitis herpetiformis (DH) is a very itchy rash consisting of bumps and blisters. The rash is chronic (long-term).
Causes
DH usually begins in people age 40 and older. Children can sometimes be affected. It occurs in both men and women.
The exact cause is unknown. Despite the name, it is not related to the herpes virus. DH is an autoimmune disorder. There is a strong link between DH and celiac disease. Celiac disease is an autoimmune disorder that causes inflammation in the small intestine from eating gluten. People with DH also have a sensitivity to gluten, which causes the skin rash. About 20% of people with celiac disease also have DH.
Symptoms
Symptoms include:
- Extremely itchy bumps or blisters, most often on the elbows, knees, back, and buttocks.
- Rashes that are usually the same size and shape on both sides.
- The rash can look like eczema.
- Scratch marks and skin erosions instead of blisters in some people.
Most people with DH have damage to their intestines from eating gluten. But only some have intestinal symptoms.
Exams and Tests
In most cases, a skin biopsy and direct immunofluorescence test of the skin are performed. Your health care provider may also recommend a biopsy of the intestines. Blood tests may be ordered to support the diagnosis.
Treatment
An antibiotic called dapsone is very effective.
A strict gluten-free diet will also be recommended to help control the disease. Sticking to this diet may eliminate the need for medicines and prevent later complications.
Medicines that suppress the immune system may be used, but are less effective.
Outlook (Prognosis)
The disease may be well-controlled with treatment. Without treatment, there may be a significant risk of intestinal cancer.
Possible Complications
Complications may include:
- Autoimmune thyroid disease
- Certain cancers, especially lymphomas of the intestines
- Side effects of the medicines used to treat DH
When to Contact a Medical Professional
Contact your provider if you have a rash that continues despite treatment.
Prevention
There is no known prevention of this disease. People with this condition may be able to prevent complications by avoiding foods that contain gluten.
Alternative Names
Duhring disease; DH
References
James WD. Chronic blistering dermatoses. In: James WD, ed. Andrews' Diseases of the Skin: Clinical Dermatology. 14th ed. Philadelphia, PA: Elsevier; 2026:chap 16.
Lebwohl B, Green PHR. Celiac disease. In: Feldman M, Friedman LS, Brandt LJ, eds. Sleisenger and Fordtran's Gastrointestinal and Liver Disease. 11th ed. Philadelphia, PA: Elsevier; 2021:chap 107.
Shields BE, Hull CM, Zone JJ. Dermatitis herpetiformis and linear IgA bullous dermatosis. In: Bolognia JL, Schaffer JV, Cerroni L, eds. Dermatology. 5th ed. Philadelphia, PA: Elsevier; 2025:chap 31.
Review Date 6/3/2025
Updated by: Ramin Fathi, MD, FAAD, Director, Phoenix Surgical Dermatology Group, Phoenix, AZ. Also reviewed by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.